Overview
Birth control is any method used to prevent pregnancy. Another word for birth control is contraception.
If you have sex without birth control, there is a chance that you could get pregnant. This is true even if you have not started having periods yet or you are getting close to menopause.
The only sure way to prevent pregnancy is to not have sex. But finding a good method of birth control that you are comfortable with can help you avoid an unplanned pregnancy.
Be sure to tell your healthcare provider about any health problems you have or medicines you take. They can help you choose the birth control method that is right for you.
Types of Birth Control
There are many kinds of birth control. Each has pros and cons. Find what works for you.
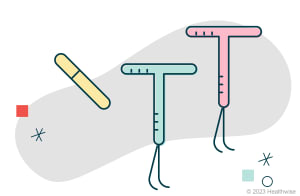
Long-acting reversible contraception (LARC). These are placed inside your body by a healthcare provider. They can prevent pregnancy for years.
Examples include:
- An implant (hormonal).
- Copper intrauterine device (IUD).
- Hormonal IUDs.
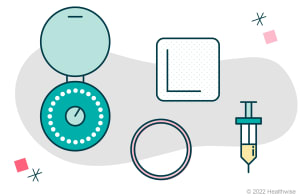
Short-acting hormonal methods. These release hormones (estrogen and progestin, or progestin only).
Examples include:

Barrier methods. Use these every time you have vaginal sex.
Examples include:
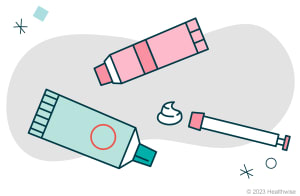
Spermicides. These kill sperm or stop sperm from moving. They can be a gel, cream, foam, film, or tablet. Use them before vaginal sex. An example is nonoxynol-9.

Fertility awareness. You'll learn when you're most likely to become pregnant (fertile). You can avoid vaginal sex at that time.
It's also called:
- Natural family planning.
- The rhythm method.

Permanent birth control (sterilization). This can be an option if you're sure that you don't want to get pregnant later.
This includes:
Emergency contraception. This is a backup method. Use it if you didn't use birth control or your birth control method failed.
Examples include:
- Copper IUDs.
- Emergency contraceptive pills.
Birth control following pregnancy
Talk to your healthcare provider about the options for birth control after your delivery. They include implants and intrauterine devices (IUDs), hormonal methods, and barrier methods. Many types of birth control are safe to use if you're going to breastfeed. But some work better than others.
Learn more
Watch
Choosing a Birth Control Method
Before you choose birth control, you might think about:

How well it works.
- Some types work better than others to prevent pregnancy.
- Think about how important it is for you to not get pregnant.
How easy it is to use.
- Some types are taken daily.
- Other types are used each time you have vaginal sex.
- Others work for years without you having to do anything.
- For some, you'll avoid vaginal sex at certain times.
How much it costs.
- Some types are free in some clinics.
- Other types cost a lot at first but work for years.
- Provincial health plans or private health insurance may cover prescription birth control.
Whether it protects you from sexually transmitted infections (STIs).
- Condoms can help protect you.
Whether it uses hormones.
- Some release estrogen and progestin. Some release progestin only.
- There are many choices, such as pills, patches, a ring, or IUDs.
If you want to get pregnant later.
- Some types allow you to get pregnant soon after you stop taking them.
- It may take months to become fertile again after stopping other types.
- Some types are meant to be permanent.

How easy it is to get.
- Some types are placed by a healthcare provider.
- Others need a prescription.
- Some are available over the counter (OTC).

Privacy.
- Some types are easier to keep private.
- Others need to be used often and may be less private.
How it fits into your life.
- Some types interrupt sex.
- After other types are placed, you don't have to do anything.
- For some types, you'll avoid vaginal sex at certain times of your menstrual cycle.

If you have health problems.
- You may not be able to use certain types if you:
- Smoke.
- Just had a baby.
- Have had breast cancer.
- Some types may help with acne or period problems, such as heavy bleeding.
Time and effort to use
Birth control must be used correctly in order to prevent pregnancy. When you decide which birth control method to use, be honest about how much effort you are willing to put into birth control. If you aren't comfortable with or might not consistently use a birth control method for any reason, that method isn't likely to be reliable for you in the long run.
Some birth control methods require more effort than others.
- Long-acting reversible contraception (LARC) (such as implants, hormonal IUDs, and copper IUDs) works to prevent pregnancy for 3 to 10 years. Talk to your healthcare provider about how long you can use it. After it's in place, you don't need to do anything.
- Barrier methods (including the diaphragm; cervical cap; male condom; female condom; and spermicidal foam, sponge, gel, suppository, or film) can interrupt sex. And you have to use them every time you have sex. Diaphragms and cervical caps are not widely available in Canada. Buying the necessary spermicidal jelly to use with them is difficult.
- Combination pills are taken each day. Progestin-only pills must be taken at the same time each day. If you miss a pill, you'll need to use a backup birth control method.
- Patches are replaced 3 times each month.
- Vaginal rings are inserted into the vagina 1 time each month.
- Fertility awareness requires that a couple chart the time during a woman's menstrual cycle when she is most likely to become pregnant. The couple must avoid intercourse or use a barrier method during that time.
- Sterilization is a surgical procedure. It's done for men or women who decide that they don't want to have any (or more) children. It's intended to be permanent.
Health issues that might limit your choices
If you have health problems or other risk factors, some birth control methods may not be safe for you. To make sure a method is right for you, your healthcare provider will need to know if you:
- Smoke. If you smoke more than 15 cigarettes a day and are 35 or older or have high blood pressure, a history of stroke, a history of blood clots, liver disease, or heart disease, you may not be able to use combined hormonal methods.
- Have any serious health problems, such as heart disease, high blood pressure, diabetes, or migraine headaches.
- Have had blood clots in the legs (deep vein thrombosis) or lungs (pulmonary embolism), or have a close family member who had blood clots in the legs or lungs.
- Are pregnant.
- Have just delivered a baby. If you just had a baby, the estrogen-progestin methods of birth control aren't recommended in the first few weeks.
- Have breast cancer or a history of breast cancer.
- Have a sexually transmitted infection (STI).
Learn more
Emergency Contraception
Emergency contraception is a way to prevent pregnancy if:
- you’ve had unprotected sex
- you’ve been sexually assaulted
- used the withdrawal (pulling out) method
- a condom broke, leaked, slipped, or fell off
- your method of birth control wasn’t used the right way, or you are taking other medicines that may affect your birth control
The most effective emergency contraception is prescribed by a healthcare provider. This includes the copper IUD (inserted by a healthcare provider) or a prescription pill. You can get emergency contraceptive pills (morning-after pills or plan B) without a prescription at most drugstores and sexual health clinics.
If you have unprotected sex, use EC as soon as possible. If you are already pregnant and use EC pills, they will not stop a pregnancy. Emergency contraception does not protect against sexually transmitted infections.
Learn more
How to Get Birth Control
- You can buy:
- Condoms, sponges, and spermicides without a prescription in drugstores, online, and in many grocery stores.
- Some forms of emergency contraception without a prescription at most drugstores and sexual health clinics.
- You need to see a healthcare provider or visit a sexual health clinic to:
- Get a prescription for birth control pills and other methods that use hormones.
- Have an implant or IUD inserted, including the type of IUD used for emergency contraception.
- Get a hormone shot.
- Get a prescription for a diaphragm or cervical cap. Diaphragms and cervical caps are not widely available in Canada. Buying the necessary spermicidal jelly to use with them is difficult.
- Get a prescription for certain kinds of emergency contraception.
When to Call a Doctor
Call 911 or other emergency services if you have:
- Sudden, severe chest pain.
- Difficulty breathing.
- Sudden, severe headache.
Call your healthcare provider now if you:
- Have severe pain in your belly.
- Have headaches that:
- Happen more often.
- Are getting worse.
- Start with auras, such as seeing spots, wavy lines, or flashing lights. Your hands, arms, or face may tingle or feel numb.
- Have signs of a blood clot, such as:
- Pain in your calf, back of the knee, thigh, or groin.
- Redness and swelling in your leg or groin.
- Feel depressed.
- Have heavy or prolonged bleeding.
- Think you may be pregnant.
- Notice yellowing of your skin or eyes.
It's common to have mild headaches, mild nausea, mild breast tenderness, or irregular bleeding (spotting) when starting birth control. These mild symptoms should improve over time. If you have problems with a birth control method, talk with your healthcare provider. They may recommend another birth control method or help you solve the problem you are having.
References
Citations
- Thaxton L, Lavelanet A (2019). Systematic review of efficacy with extending contraceptive implant duration. International Journal of Gynaecology and Obstetrics: The Official Organ of the International Federation of Gynaecology and Obstetrics, 144(1): 2–8. DOI: 10.1002/ijgo.12696. Accessed December 7, 2022.
- Ti AJ, et al. (2020). Effectiveness and safety of extending intrauterine device duration: A systematic review. American Journal of Obstetrics and Gynecology, 223(1): 24–35.e3. DOI: 10.1016/j.ajog.2020.01.014. Accessed August 29, 2022.
Credits
Adaptation Date: 7/12/2024
Adapted By: Alberta Health Services
Adaptation Reviewed By: Alberta Health Services
Thaxton L, Lavelanet A (2019). Systematic review of efficacy with extending contraceptive implant duration. International Journal of Gynaecology and Obstetrics: The Official Organ of the International Federation of Gynaecology and Obstetrics, 144(1): 2–8. DOI: 10.1002/ijgo.12696. Accessed December 7, 2022.
Ti AJ, et al. (2020). Effectiveness and safety of extending intrauterine device duration: A systematic review. American Journal of Obstetrics and Gynecology, 223(1): 24–35.e3. DOI: 10.1016/j.ajog.2020.01.014. Accessed August 29, 2022.